Vaccine-Preventable Diseases (VPDs) and Respiratory Diseases

Program Overview
The State of Nevada, Vaccine-Preventable Disease (VPD) and Respiratory Disease Program’s goal is to enhance outbreak surveillance by building upon established surveillance systems to provide more complete and representative data to inform new public health approaches and strengthen surveillance protocols for VPDs. Enhancing surveillance in Nevada includes working on the timely detection of VPDs and respiratory diseases, efficient analysis of disease trends, and management of outbreaks.
Detailed descriptions and resources for VPDs and respiratory diseases are available in their respective sections. The Office of State Epidemiology webpage, provides information on how to report a case and includes a complete list of all Nevada Reportable Diseases within the Confidential Morbidity Report Form.
The VPD and respiratory diseases program currently focuses on the following diseases:
- Acute flaccid myelitis (AFM),
- Coronavirus (COVID-19)
- Influenza (Flu),
- Measles
- Meningococcal disease (focusing on disease causing serogroups B, C, and Y),
- Pertussis (whooping cough),
- Respiratory syncytial virus (RSV)
- Varicella (chicken pox).
Acute Flaccid Myelitis (AFM)

What is Acute Flaccid Myelitis (AFM)?
Acute flaccid myelitis (AFM) is an uncommon but serious neurologic condition. It affects the nervous system, specifically the area of the spinal cord called gray matter, causing the muscles and reflexes in the body to become weak.
The U.S. has seen increases in AFM cases occurring in 2014, 2016, and 2018. Most AFM cases (more than 90%) have been in young children between the ages of 4 and 6 years old.
Symptoms
The most common symptoms of AFM are:
- Sudden onset of arm or leg weakness
- Loss of muscle tone
- Loss of reflexes
Causes
AFM can be caused by viruses, including enteroviruses. Enteroviruses are common and usually cause mild illness. AFM can also be caused by other viruses, including flaviviruses (West Nile virus, Japanese encephalitis virus), herpesviruses, and adenoviruses.
For more information on what causes AFM, navigate to the CDC website.
Prevention
It is not currently known what triggers AFM in a person, so there is no specific action to take to prevent AFM. However, you can take steps to prevent getting sick with a virus that may cause AFM – Preventing AFM.
To lower yours and your child’s risk of getting a virus that may cause AFM:
- Wash your hands often with soap and water for at least 20 seconds.
- Avoid touching your face with unwashed hands.
- Avoid close contact with people who are sick.
- Stay up to date on recommended vaccinations.
You can lower the chance of spreading a virus by:
- Clean and disinfect frequently touched surfaces, like toys, mobile devices, and doorknobs.
- Cover coughs and sneezes with a tissue or upper shirt sleeve, not hands.
- Stay at home if you or your child are sick.
Testing and Diagnosis
It is important that the tests to help with diagnosis are done as soon as possible after a patient develops symptoms.
Clinicians diagnose AFM by taking a thorough medical history, doing a physical exam, and performing an MRI to review pictures of the spinal cord.
The CDC asks that we monitor our state for any AFM cases and are actively increasing surveillance. This is to better understand the disease and devise ways to prevent it. You can find more about testing and diagnosis for AFM here.
Immunizations
There is currently no immunization that an individual can receive to prevent AFM. In 2014, the term AFM was adopted to describe poliomyelitis without a known cause and not caused by poliovirus. AFM has some similarities with polio, such as lesions in the great matter of the spinal cord and flaccid limb weakness that can result in paralysis. Polio can be prevented by a vaccine.
Where can I find more information about acute flaccid myelitis?
Resources in Nevada:
DPBH – Epidemiology and Laboratory Capacity (ELC)
Acute Flaccid Myelitis: Alert for Healthcare Providers
National Resources:
The Centers for Disease Control and Prevention (CDC) – Acute Flaccid Myelitis
Acute Flaccid Myelitis Association
Coronavirus Diseases (COVID-19)
What is SARS-CoV-2 (COVID-19)?
COVID-19 is caused by infection with the SARS-CoV-2 virus and most often causes respiratory symptoms similar to those of a cold, the flu, or pneumonia. However, it can affect more than your lungs and respiratory system; other parts of your body may also be impacted by the disease. While most people with COVID-19 have mild symptoms, some people may become severely ill.
Signs and Symptoms
The following list does not include all possible symptoms of COVID-19. It is possible symptoms may change depending on the COVID-19 variants and can vary depending on a person’s vaccination status. Possible symptoms include:
- Fever or chills
- Cough
- Shortness of breath or difficulty breathing
- Sore throat
- Congestion or runny nose
- New loss of taste or smell
- Fatigue
- Muscle or body aches
- Headache
- Nausea or vomiting
- Diarrhea
Risk factors for severe illness from COVID-19
Some people are more likely to get very sick if they get COVID-19. This includes people who:
- Are older
- Are immunocompromised (meaning have a weakened immune system)
- Have certain disabilities or
- Have underlying health conditions
Differences Between Flu and COVID-19
Influenza and COVID-19 are both contagious respiratory illnesses, but they are caused by different viruses. COVID-19 is caused by infection with the coronavirus called SARS-CoV-2, and flu is caused by infection with one of the influenza viruses. You cannot tell the difference between flu and COVID-19 by symptoms alone because some of the symptoms are the same. To figure out if you might have COVID-19, you can take an at-home test or see a healthcare provider to get tested.
How COVID-19 Spreads
COVID-19 can spread when an infected person breathes out droplets and very small particles that contain the virus. This can result in other people breathing in these droplets and particles, or the droplets or particles landing on others’ eyes, nose, or mouth. In other cases, these droplets may contaminate the surfaces they touch.
It is important to note that anyone infected with COVID-19 can spread it, even if they do NOT have any symptoms. In some situations, it can be spread even from people to animals.
Prevention
There are a few different actions that you can take to help protect yourself, your household, and people within your community from COVID-19.
You can prevent COVID-19 and other respiratory viruses by:
- Staying up-to-date with your immunizations
- Practicing proper hygiene for respiratory virus prevention
- Taking steps for cleaner air for respiratory virus prevention (bringing in fresh outside air, purifying indoor air, or gathering outdoors).
- Wearing masks to reduce risk of spreading respiratory virus
- Physical distancing between yourself and others
- Testing for respiratory viruses
Where can I find more information on COVID-19 and vaccinations?
Resources in Nevada:
Nevada 211 – COVID-19 Resources
Southern Nevada Health District – COVID-19 Resources
National Resources:
Health and Human Services – Coronavirus (COVID-19)
Getting Your COVID-19 Vaccine – CDC
Recent Trends for COVID-19 can be found by navigating to this page.
Influenza

What is influenza?
Influenza, also known as “flu,” is a contagious respiratory illness caused by influenza viruses. It can cause mild to severe illness and at times can lead to hospitalization and death.
Symptoms
Flu symptoms usually come on suddenly. People who have flu often feel some or all of these signs and symptoms**:
- Fever* or feeling feverish/having chills
- Cough
- Sore throat
- Runny or stuffy nose
- Muscle or body aches
- Headaches
- Fatigue (tiredness)
- Some people may have vomiting and diarrhea, though this is more common in children than adults.
*Important to note that not everyone with the flu will have a fever.
**If you develop flu-like symptoms and you’ve had recent contact with a sick or dead animal, contact your healthcare provider and let them know about the animal contact.
Flu Complications
Most people who get the flu will recover in a few days to less than two weeks, but some people can develop complications (such a pneumonia) because of flu, some of which may be life-threatening and result in death.
People at Higher Risk from Flu
Anyone can become sick with the flu, even healthy people, and serious problems related to the flu can happen to anyone at any age, but some people are at higher risk of developing serious flu-related complications if they get sick. This includes people:
- 65 years and older
- People of any age with certain chronic medical conditions (such as asthma, diabetes or heart disease)
- Pregnant people and children younger than 5 years but especially those younger than 2 years old
Diagnosis
A number of tests are available to detect influenza viruses. For more information click here.
The Difference Between Flu and COVID-19
Flu and COVID-19 are both contagious respiratory illnesses, but they are caused by different viruses. Flu and COVID-19 can cause many of the same symptoms. COVID-19 can cause more severe illness in some people and some people infected with SARS-CoV-2 may take longer to show symptoms and may be contagious for longer periods of time. For more information click here.
The Difference Between Cold and Flu
Flu and the common cold are both respiratory illnesses, but they are caused by different viruses. The flu is caused by influenza viruses only, whereas the common cold can be caused by several different viruses, including rhinoviruses, parainfluenza, and seasonal coronaviruses (not COVID-19). The cold and flu are known to have similar symptoms but in general the flu is worse than the common cold because symptoms are more intense and can begin abruptly. For more information click here.
Preventing Seasonal Flu
The best way to reduce your risk from seasonal flu and its potentially serious complications is to get a flu vaccine every year. For more information on if the flu vaccine is right for you click here. In addition to getting vaccinated, it is important to take actions daily to help stop the spread of germs by:
- Covering coughs and sneezes
- Washing your hands often with soap and water. If soap and water are not available, use an alcohol-based hand rub.
- Avoiding touching your eyes, nose, and mouth. Germs spread this way.
- Improving air quality by bringing in fresh outside air, purifying indoor air, or gathering outdoors. Cleaner air can reduce the risk of exposure to viruses.

CDC’s respiratory virus guidance that consists of 5 core and 3 additional prevention strategies.
Where can I find more information on influenza and vaccination?
Resources in Nevada:
Flu Resources – Southern Nevada Health District
Influenza (“Flu”) Flu Season Information – Northern Nevada Public Health
Flu Shots Available – Nevada Department of Veterans Services
Flu Shots Pregnancy Guidance – Nevada State Immunization Program
National Resources:
Association of Immunization Managers – Flu Resources
National Foundation for Infectious Diseases – Flu
Recent Trends for influenza can be found by navigating to this page.
Measles
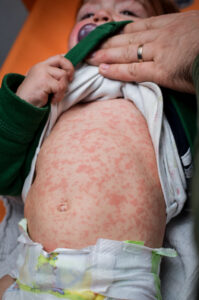
What is Measles (Rubeola)?
Measles is a highly contagious viral infection and can be very serious. About 9 in 10 people without immunity (via vaccination or previous infection) who come into close contact with someone with measles will get it.
This disease is known to be spread through the air by respiratory droplets that are produced through coughing or sneezing.
Signs and symptoms
It is important to seek care immediately if you suspect you or your child have been exposed to measles. Symptoms usually appear within 7-14 days after exposure to the virus and include:
- Fever (may spike to over 104˚)
- Cough (develops in the early stages of infection)
- Runny nose (also known as coryza)
- Red, watery eyes (also known as conjunctivitis)
- Koplik spots (small white spots that appear inside the cheeks 2-3 days after symptoms begin)
- Rash (red, blotchy rash that usually appears 3-5 days after first symptoms. Typically, this rash starts on the face and upper body, then spreads to the trunk, hands, and feet).
Complications
Measles can cause serious health complications, especially in children under 5, adults over 20, pregnant people, and people with weakened immune systems. Complications include:
- Ear infections
- Diarrhea
Severe complications in children and adults include:
- Hospitalization – which occurs in about 1 in 5 unvaccinated people in the U.S. who get measles
- Pneumonia – as many as 1 out of every 20 children with measles gets pneumonia
- Encephalitis – 1 child out of every 1,000 who get measles will develop encephalitis (swelling of the brain)
- Death – nearly 1 to 3 of every 1,000 children who become infected with measles will die from respiratory and neurologic complications
- Complications during pregnancy – if you are pregnant and have not had the MMR vaccine it is possible that measles will cause a premature birth or increase the chances of the infant having a low birthweight.
Long term complications:
- Subacute sclerosing panencephalitis (SSPE) which is rare but fatal disease of the central nervous system. It is a result of a measles virus infection acquired earlier in life.
Prevention
The best way to be protected against measles is to receive the measles, mumps, and rubella (MMR) vaccine. Children may get 2 doses of MMRV (measles, mumps, rubella, and varicella) vaccine instead. Both the MMR and MMRV vaccines are safe and effective. They usually protect people for life against measles and rubella; but immunity against mumps and varicella may decrease over time. It is recommended by doctors that children receive two doses of either of these vaccines as the best way to protect against the virus.
To read more information on when your child should be vaccinated, please click here.
Where can I find more information on measles and vaccination?
Resources in Nevada:
The Office of State Epidemiology
Southern Nevada Health District – Measles
National Resources:
Centers for Disease Control and Prevention – Measles
Office of Human Services Emergency Preparedness and Response – Measles
Meningococcal Disease

What is meningococcal disease?
Meningococcal disease is a name for any infection caused by the bacteria called Neisseria meningitidis. The two most common types of meningococcal infections are meningitis and bloodstream infections.
Meningococcal meningitis happens when the Neisseria meningitidis bacteria infect the lining of the brain and spinal cord and cause swelling.
Meningococcal bloodstream infections happen when the Neisseria meningitidis bacteria enter the blood and damage the walls of the blood vessels. This causes bleeding in the skin and organs.
Symptoms
The most common symptoms of meningococcal meningitis include:
- Fever
- Headache
- Stiff neck
Additional symptoms may include:
- Altered mental status (confusion)
- Nausea
- Photophobia (eyes being more sensitive to light)
- Vomiting
Symptoms in infants:
Infants may not have the classic symptoms listed above. If they do, it may be difficult to notice the symptoms.
Instead, infants may
- Appear to be slow or inactive
- Be irritable
- Feed poorly
- Have a bulging anterior fontanelle (the soft spot of the skull)
- Have abnormal reflexes
- Vomit
Bloodstream infection
Symptoms of a meningococcal bloodstream infection may include:
- Cold hands and feet
- Diarrhea or nausea with or without vomiting
- Fatigue (feeling tired)
- Fever and chills
- Rapid breathing
- Severe aches or pain in the muscles, joints, chest, or abdomen (belly)
- In the later stages, a dark purple rash
Risk Factors
Factors that increase the risk for meningococcal disease include:
- Age
- Certain medical conditions
- Certain medicines
- Close or lengthy contact with someone with meningococcal disease
- Certain places and settings where people work, live, and travel where there is a higher risk of transmission
Prevention
Vaccination
The best way to prevent meningococcal disease is to get vaccinated. The CDC recommends meningococcal vaccination for:
- All preteen and teens
- Children and adults at increased risk for meningococcal disease
Where can I find more information about meningococcal disease and vaccinations?
Resources in Nevada:
Meningitis Vaccine Requirement for 12th Graders
Vaccine Preventable Diseases – Meningococcal
Southern Nevada Health District – Meningococcal Disease
National Resources:
Centers for Disease Control and Prevention (CDC) Educational materials on meningococcal disease
Centers for Disease Control and Prevention (CDC) Cochlear implants and vaccine recommendations
Pertussis (Whooping Cough)
What is Pertussis?
Pertussis also known as whooping cough, is a respiratory illness caused by a type of bacteria called Bordetella pertussis, which is only found in humans.
How it Spreads
Pertussis, also known as whooping cough, is primarily spread through the air when an infected person coughs or sneezes. Within this route of transmission, the release of tiny droplets occur that contain the bacteria that then can be inhaled by others nearby. Thus, spreading through the respiratory droplets from the nose and throat of an infected individual.
Proximity with an infected individual can also increase the risk of catching pertussis.
There is also a potential for indirect transmission. This transmission is less common, but it is possible for pertussis to spread by touching contaminated surfaces and then touching your eyes, mouth, or nose.
Symptoms
Symptoms of Pertussis usually take 5 to 10 days to appear after exposure to the bacteria that causes it. It could take up to 3 weeks for symptoms to appear.
Appears like a common cold.
Pertussis or (whooping cough) will appear similar to a common cold early on. Healthcare providers often do not suspect or diagnose the disease until more severe symptoms appear.
Early symptoms can last for 1 to 2 weeks and usually include:
- Runny or stuffy nose
- Low-grade fever (less than 100.4˚F)
- Mild, occasional cough
Infants may struggle to breathe.
Many infants with whooping cough don’t actually cough. Instead, they may have apnea– pauses in breathing that can be life-threatening. This apnea may cause cyanosis (blue or purple discoloration of the skin) or they may struggle to breathe. In some cases, whooping cough may seem like a common cold for the entire illness.
Later symptoms
Rapid, violent, and uncontrolled coughing fits
Around one to two weeks after the first symptoms start, people may develop paroxysms, or coughing fits. These coughing fits can usually last between 1 to 6 weeks but sometimes persist for up to 10 weeks. The cough will generally get worse and becomes more common as the illness progresses.
Coughing fits can cause people to
- Make a high-pitched “whoop” when they inhale after a coughing fit
- Vomit during or after coughing fits
- Feel very tired after the fit, but usually seem well in-between fits
- Have difficulty sleeping at night
- Struggle to breathe
- Fracture (break) a rib
Recovery can be slow with the cough becoming milder and less common over time.
Complications
Whooping cough can cause serious and sometimes deadly complications in infants and young children, especially those who have not received all recommended whooping cough vaccinations.
It is important to note that serious complications are common. About 1 in 3 infants younger than one year old who contract whooping cough require hospital care. The younger the infant, the more likely they’ll need hospital treatment.
Infants younger than one year old who are treated in the hospital can have:
- Apnea: 2 in 3 (68%)
- Pneumonia (lung infection): 1 in 5 (22%)
- Convulsions (violent, uncontrolled shaking): 1 in 50 (2%)
- Encephalopathy (disease of the brain) 1 in 150 (0.6%)
One in 100 (1%) will die from their complications.
It is also important to note that teens and adults can also have complications, like pneumonia, from whooping cough. The complications are usually less serious in this older age group, especially in those who have been vaccinated against whooping cough. However, if the complications are serious, some people may need care in the hospital.
Vaccination
Whooping cough vaccines are the best way to protect against whooping cough. These vaccines are effective, however there are incidences of break-through cases that occur. For any cases in individuals who have been vaccinated, the illness is generally milder.
To find more information regarding the whooping cough vaccination, please click here.
Where can I find more information on pertussis and vaccination?
Resources in Nevada:
Southern Nevada Health District – Pertussis (Whooping Cough)
Nevada State Immunization Program – Cocooning Program
Northern Nevada Public Health – Pertussis Information
National Resources:
Centers for Disease Control and Prevention – Whooping Cough
Respiratory Syncytial Virus (RSV)

What is Respiratory Syncytial Virus (RSV)?
Respiratory syncytial virus, or RSV, is a common respiratory virus that infects the nose, throat, and lungs. RSV symptoms make it difficult to distinguish it from the common cold or other respiratory viruses (like the flu or COVID-19). RSV spreads in the fall and winter seasons along with other respiratory viruses. It usually peaks in December and January.
Who is at risk?
RSV does not usually cause severe illness in healthy adults and children. However, older adults and infants younger than 6 months of age can become very sick if infected and may need to be hospitalized.
RSV can potentially cause more severe illness such as bronchiolitis (inflammation of the small airways in the lungs) and pneumonia (infection of the lungs). It is noted to be the most common cause of bronchiolitis and pneumonia in children younger than one year of age.
How it Spreads
Respiratory Syncytial Virus (RSV) has a few different modes of transmission. The most common mode being through respiratory droplet spread which can be released when an infected person coughs or sneezes, which can be inhaled directly.
The virus can also survive on surfaces like countertops and toys for up to several hours so touching a contaminated surface and then touching your face can lead to infection.
Prevention
Immunization for Infants:
- The CDC recommends that all babies be protected from severe RSV by one of two immunization options: A maternal RSV vaccine given to the mother during pregnancy, or an RSV antibody given to your baby. Most babies do not need both.
- The maternal RSV vaccine is given during weeks 32 through 35 of pregnancy. Maternal antibodies protect the baby against RSV for approximately 6 months after birth.
- An RSV antibody (nirsevimab) can be given to babies and some young children. This antibody provides immediate protection against RSV and lasts at least 5 months.
For more information on RSV infant immunizations, please click here.
Immunization for Older Adults:
- RSV can be dangerous for older adults, especially those who have certain medical conditions, are elderly or frail, or live in a nursing home.
- CDC recommends that everyone ages 75 and older get an RSV vaccine.
- CDC recommends adults ages 60-74 who are at increased risk of severe RSV disease get an RSV vaccine.
For more information on RSV immunization for older adults, please click here.
Other Prevention Strategies:
Along with immunizations other core prevention strategies include: practicing good hygiene, taking steps to improve air quality, seeking out treatment if you believe you have a respiratory virus, and staying at home to prevent the spread.
Additional prevention strategies that are also helpful is to wear a mask, practice social distancing, and taking tests to be sure you have a respiratory virus.
It is important to make sure you stay home and away from others until your symptoms have gotten better and you are fever free without the use of medicine for at least 24 hours. Then make sure to take extra precautions for the next 5 days as you recover.
Where can I find more information on RSV and vaccinations?
Resources in Nevada:
RSV – Northern Nevada Public Health
RSV (Respiratory Syncytial Virus) – Office of State Epidemiology
RSV Prevention for Infants – Nevada State Immunization Program
RSV 60+ – Nevada State Immunization Program
National Resources:
Varicella

What is Chickenpox (Varicella)?
Chickenpox is a highly contagious disease caused by the varicella-zoster virus (VZV). The virus spreads mainly through close contact with someone who has chickenpox. The predominant symptom is an itchy, blister-like rash. Additional symptoms include: low-grade fever, tiredness, headache, loss of appetite, coughing, and stomachache. Chickenpox illness usually lasts about 4 to 7 days. The best way to prevent chickenpox is to get the chickenpox vaccine.
It is important to note that chickenpox and shingles are both caused by the varicella-zoster virus and after an individual has chickenpox, the virus remains dormant in the body and can reactivate later in life as shingles. Shingles is also more common in people with weakened immune systems and people over 50 years of age.
Signs and Symptoms
The classic symptom of chickenpox is a rash that turns into itchy, fluid-filled blisters that eventually turn into scabs. The rash may first show up on the chest, back, and face, before it spreads to the rest of the body. A person with chickenpox may have as many as 500 blisters. It usually takes about 1 week for all blisters to become scabs.
Who is at risk?
Anyone who has not had chickenpox or received the chickenpox vaccine is at higher risk of getting the disease.
Some people who get chickenpox may have more severe symptoms and may be at higher risk for complications. Chickenpox can be serious, and in rare circumstances, life-threatening, for many individuals.
Some people who have been vaccinated against chickenpox can still get the disease. However, they usually have milder symptoms and shorter illness than people who are not vaccinated.
How it Spreads
Contact with someone with chickenpox
Chickenpox is a highly contagious disease caused by varicella-zoster virus (VZV). It mainly spreads from unvaccinated people with chickenpox to others who have never been infected with the virus. Up to 90% of people who are not immune and have close contact with someone with chickenpox will also get infected.
A person with chickenpox is contagious 1 to 2 days before the rash begins, until all the chickenpox lesions have crusted (scabbed over).
If a vaccinated person gets the disease, they can still spread it to others. Vaccinated people who get chickenpox may develop lesions that do not crust. These people are contagious until no new lesions have appeared for 24 hours.
Contact with someone with shingles
VZV also causes shingles. After people recover from chickenpox, the virus remains dormant in the body. People get shingles if VZV reactivates in their bodies later in life.
People who never had chickenpox or didn’t get chickenpox vaccine can get infected with VZV from someone who has shingles. They will develop chickenpox, not shingles. These people can get the virus through:
- Direct contact with the fluid from shingles rash blisters.
- Breathing in virus particles that come from the blisters.
It takes about 2 weeks (10 to 21 days) after exposure to a person with chickenpox or shingles for someone to develop chickenpox.
Prevention
Protect yourself with the vaccine. The best way to prevent chickenpox is to get the chickenpox vaccine. Everyone, including children, adolescents, and adults, should get 2 doses of chickenpox vaccine if they have never had chickenpox or were never vaccinated. The varicella vaccine has shown to be safe and well tolerated given it provides protection against chickenpox with significantly milder symptoms while minimizing the risk of complications and potential transmission to vulnerable individuals whereas an infection can led to more severe complications.
Treatment and Recovery
There are a few things that you can do at home to help relieve chickenpox symptoms and prevent skin infections. Your healthcare provider can advise you on treatment options. Antiviral medication is recommended for people with chickenpox who are more likely to develop dangerous illnesses.
Reporting
Find more information about reporting a case here.
Where can I find more information about chickenpox and vaccinations?
Resources in Nevada:
Special Immunization Projects – Where to Receive Vaccines
Nevada 211 – Nevada Department of Health and Human Services.
Southern Nevada Occupational Health Center (SNOHC)
Immunization Clinic – Southern Nevada
Verification of Varicella Immunity for School and Child Care Entry
School Medical Immunization Exemption Form
National Resources:
Center for Disease Control and Prevention (CDC) Chickenpox (Varicella)
Chickenpox Vaccine Infographic (CDC) – English and Chickenpox Vaccine Infographic (CDC) – Spanish
Breakthrough Varicella Factsheet (CDC)
VPD Technical Bulletins
Increased Incidence of Measles in United States, Recommendations for Health Care Providers 4.30.2024
CDC Updated Respiratory Virus Guidance (including COVID-19) 3.07.2024
FDA Approves Use of Respiratory Syncytial Virus Vaccines (RSV) for Adults 60 and Older 9.08.2023
FDA Ends Monovalent mRNA Authorization and Simplifies Use of Bivalent COVID-19 Vaccines 4/.28.2023
Discontinuation of Reporting COVID-19 Negative Laboratory Results 3.04.2023
Bivalent COVID-19 Vaccines Now Authorized for Individuals 6 months of Age and Older 12.21.2022
RSV, Influenza and COVID-19 12.08.2022
Novavax COVID-19 Vaccine, Adjuvanted Booster Now Authorized for 18+ 9.27.2022
Data Dashboard
View Data Dashboard here.
Nevada State Immunization Program
Mission Statement
The Nevada State Immunization Program (NSIP) works with Nevada’s local health departments, hospitals, schools and clinics to facilitate vaccine distribution and programs. Our focus is ensuring equitable vaccination access across Nevada’s population. We are a trusted immunization resource and inspire a culture embracing immunization to protect to public from vaccine preventable disease.
For more information on resources, please visit the NSIP webpage.
For details about Vaccine-Preventable Diseases, click here.
To learn about School Screening data in Nevada, please navigate to this webpage.

